The second question that most people ask, in one way or another, is “what’s the prognosis?” The prognosis refers to the chance of recovery from the disease.

The prognosis, and the treatment options you have available, depends on several factors
- Whether the cancer is thymoma or thymic carcinoma.
- The type of thymoma or Thymic carcinoma.
- Whether the cancer has spread to nearby areas or other parts of the body, also referred to as the stage.
- Whether the tumor can be removed completely by surgery.
- Whether the cancer has just been diagnosed or has recurred.
- The patient’s age and overall health.
Survival statistics
Before looking at survival statistics, you should understand how these are developed and applied. Doctors use survival statistics to evaluate treatment options. Broadly, this compares the survival rates of patients taking various treatment. But there’s much more than just the treatment that has to be considered. Any factor that can impact on a patient’s prognosis needs to be taken into consideration.
These statistics are compiled from case studies and trials. Many case studies are retrospective. This means that researchers collect information from past cases, trying to draw some conclusions. The major problem with retrospective studies is that they don’t take into account new treatment and technologies.
When studies refer to survival rate, they are taken the percentage of people who are alive at a certain point in time. The most commonly used for comparison is the 5-year survival rate, the rate of people alive 5 years after their initial diagnosis.
Researches also consider all factors. For example, a study may contrast 5-year survival rates based on the stage or pathological type of the cancer.
Many studies also refer to Disease-free (DFS) and progression-free survival (PFS) rates. DFS is the number of people in complete remission after treatment. PFS is the number of people with no tumor growth or spread.
Doctors use these statistics to evaluate the prognosis
The medical community considers many cancers “cured” when doctors cannot detect cancer 5 years after diagnosis. But recurrence after 5 years is still possible.
What The Studies Show
While every case Is different, one study showed five-year survival rates of at 96% for stage I disease, 86% for stage II disease, 69% for stage III disease, and 50% for stage IV disease. In another study, the 20-year survival rates were reported as 89% for stage I disease, 91% for stage II disease, 49% for stage III disease, and 0% for stage IV disease.
Thymic carcinoma is more aggressive than thymomas, and usually not detected until it has become invasive. About 35% of people with thymic carcinoma live at least 5 years after diagnosis. Around 28% of people with thymic carcinoma live at least 10 years.
When discussing prognosis, researchers look at case studies. Each case describes the number of patients involved, and their predictive factors, such as age, stage, tumor type, etc. The conclusions drawn are general. Other case studies may result in different conclusions. In general, however, if the studies are done correctly, there should be a minimal variation.
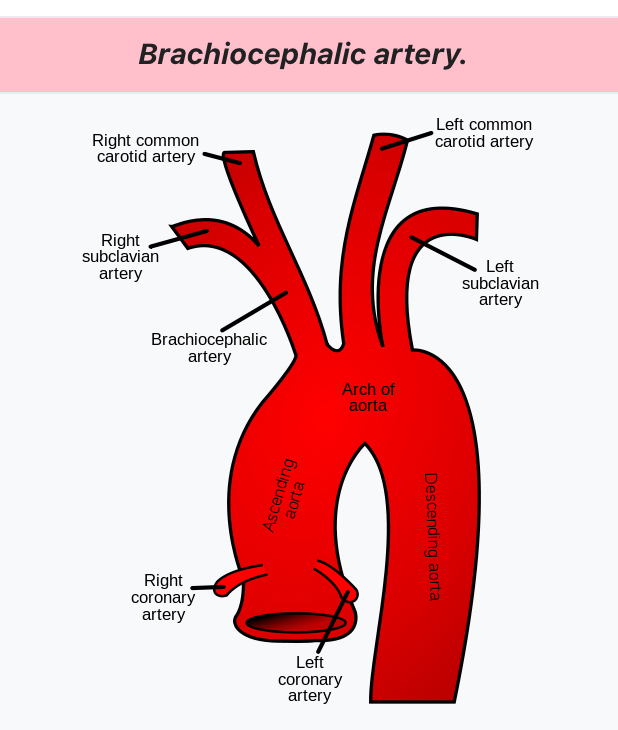
In one study, prognosis seemed connected to the invasion of the brachiocephalic artery. The brachiocephalic artery, an artery of the mediastinum that supplies blood to the right arm and the head and neck. It is the first branch of the aortic arch.
The study shown in Figure 1, from Memorial Sloan Kettering, shows 5 and 10 year survival rates based on the stage. Note that survival rates drops precipitously from stage III to IV.
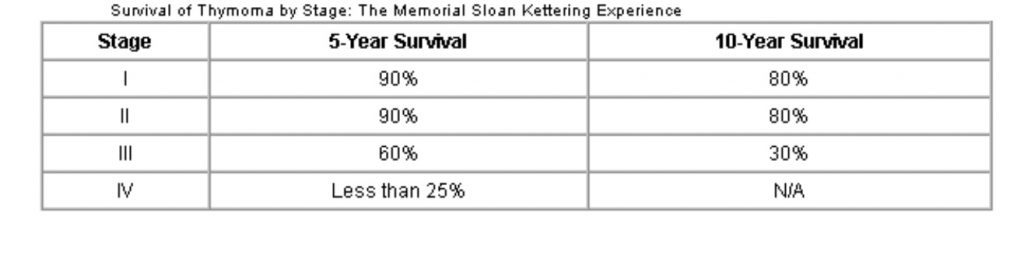

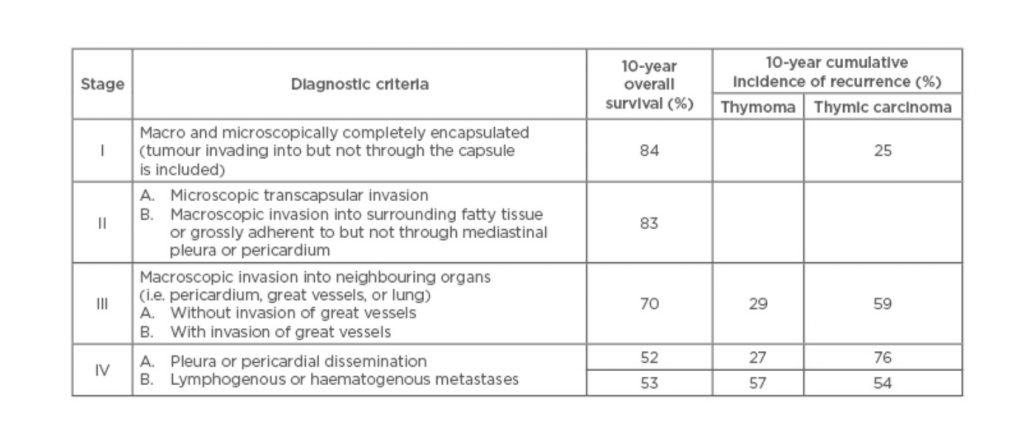
Figure 2 shows the 10-year survival rate and the incidence of recurrence:
This graph also illustrates survival probability based on stage. Again, rates drop greatly with stage over time.
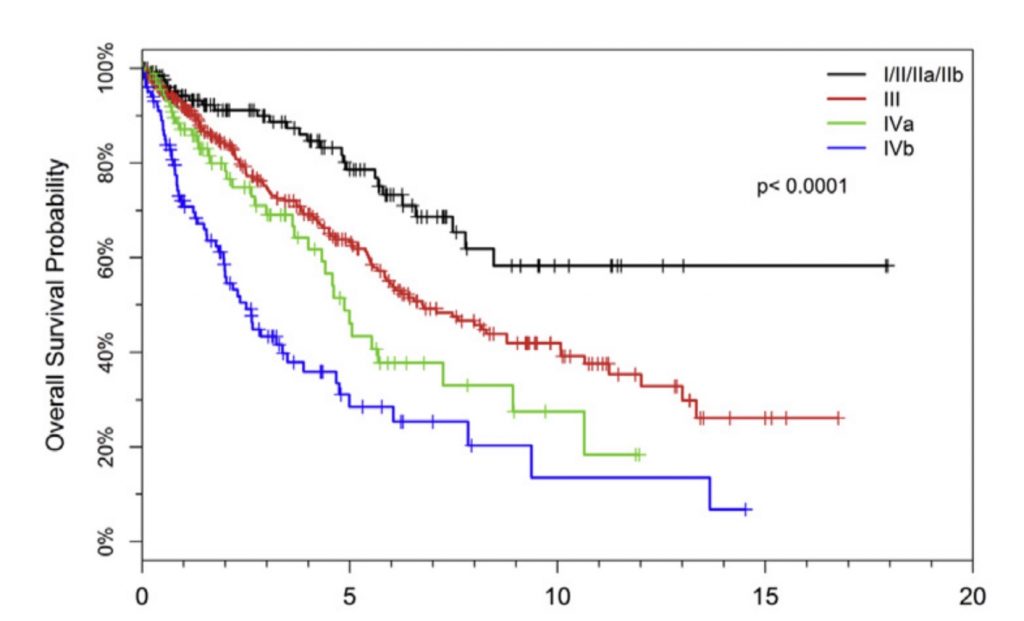
Figure 4 looks at survival rates by the classification of the tumor. The rates drop mostly with B3, well-differentiated carcinoma, and then with thymic carcinoma.

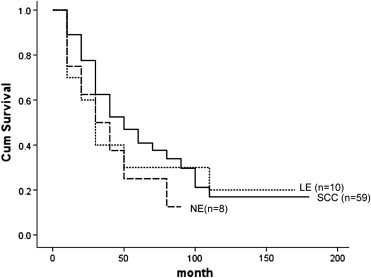
Finally, Figure 5 shows survival rates of Thymic carcinoma based on three of its many types. The numbers in parentheses on the charge represent the number of patients in the study.
SCC — Squamous cell
LE — Lymphoepithelioma-like
NE — Neuroendocrine